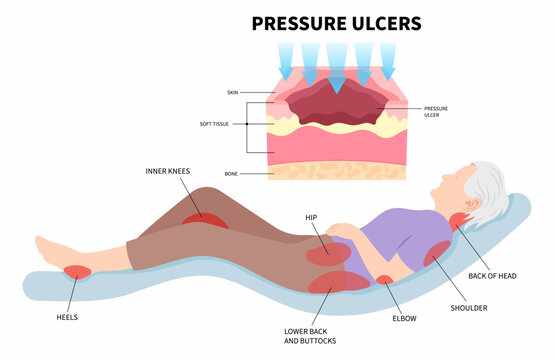
Caring for a patient with limited mobility is a journey filled with love and significant responsibilities. Looking after bedridden relatives is a common reality in Indian households. One of the most challenging aspects of this care is the prevention and management of pressure ulcers. These skin injuries occur when constant pressure on a specific area limits blood flow. Understanding the nuances of a bed sore dressing is crucial for anyone managing long-term care at home. It is not just about covering a wound; it is about creating an environment where the body can heal itself effectively.
Identifying the Stages of Skin Breakdown
Recognizing skin damage severity is vital before starting treatment. Bed sores are generally classified into stages. In the early phase, the skin might just look red or discoloured and feel warm to the touch. This is a warning sign that the tissue is under stress. As it progresses, the surface layer may break, forming a shallow open sore. In more severe cases, the damage reaches deeper into the fat, muscle, or even bone. Just as dental evaluations use X-rays for underlying structures, deep bed sores require professional assessment for internal damage. Recognizing these signs early can prevent the need for complex surgical interventions later.
The Importance of a Balanced Diet in Tissue Repair
Healing starts from the inside out. Just as patients preparing for surgery are advised to eat a nutritious diet rich in vitamins and minerals to support healing, individuals with pressure ulcers need specific nutritional support. A diet high in protein is essential for tissue repair, while calcium and vitamins C and D are vital for maintaining general health and bone strength. Staying well-hydrated is also mandatory, as dehydrated skin tears easily. Drinking plenty of water helps maintain skin turgor and washes away waste products from the cells. It is best to avoid excessive caffeine, as it can interfere with hydration levels and potentially slow down the natural recovery process.
Essential Steps for a Sterile Bed Sore Dressing
Cleanliness is the most important factor for dressing. First, wash your hands thoroughly with soap. Gently clean the wound area using a saline solution or a mild cleanser recommended by a professional. Avoid using harsh chemicals like hydrogen peroxide unless specifically told to do so, as they can damage delicate new skin cells. Once the area is clean, pat the surrounding skin dry—not the wound itself. Choosing the right dressing depends on the wound type. Some dressings provide a moist environment to speed up healing, while others are designed to absorb excess fluid. It is similar to how a dentist ensures a site is free from plaque and buildup before proceeding. Always ensure the edges of the dressing are secure but not so tight that they restrict circulation. If any medications are provided, apply them exactly as directed.
Impact of Lifestyle Habits on Skin Recovery
Small lifestyle adjustments can make a massive difference in how quickly a wound closes. For instance, if the patient smokes, it is highly recommended to stop or at least reduce the habit. Smoking narrows the blood vessels and significantly delays the healing process, increasing the risk of the wound becoming chronic. Likewise, limiting alcohol consumption is wise. Alcohol can interfere with any pain management medications or antibiotics the patient might be taking. Gentle physical activity, if the patient's condition allows, can help improve circulation. Even simple movements in bed or assisted stretches can keep the blood flowing, which is the best way to prevent new sores from forming. Consistency in these small habits creates a foundation for long-term skin health and overall patient comfort.
Maintaining Morale and Mental Well-being
Living with a chronic wound can take an emotional toll. Patients often feel a sense of loss or frustration due to their physical limitations. Much like the "insta-ready" standards on social media can make people feel inadequate about their natural appearance , a patient struggling with mobility might feel a decline in self-esteem. It is essential for caregivers to offer emotional support. Encouraging the patient and focusing on small signs of progress helps maintain a positive outlook. Every journey is unique; worth is not defined by physical mobility. A supportive home environment acts as a catalyst for physical recovery, making the technical aspects of care much more effective.
When to Seek Professional Assistance
While home care is vital, there are times when expert intervention is necessary. If you notice a foul smell, increased swelling, or if the patient develops a fever, these are signs of infection that require immediate attention. In some cases, specialized home nursing services are the best way to ensure the patient receives clinical-grade care. For families looking for specialized bed sore dressing in Nagpur, there are several qualified healthcare providers who can visit your home. They bring expertise in debridement and techniques that are difficult for laypersons. Consulting with a healthcare professional ensures the treatment plan is tailored to the specific needs of the patient.
FAQs
How often should I change a bed sore dressing? The frequency depends on the dressing type and drainage. Generally, it is changed every one to three days.
Can I use normal tap water to clean the sore? It is safer to use sterile saline or boiled and cooled water to avoid introducing bacteria into the wound.
What is the best sleeping position to avoid sores? Rotate the patient's position every two hours. Use pillows to keep bony areas like knees and ankles from touching.
Are there specific foods that help skin heal? Yes, eggs, lentils, and citrus fruits provide the protein and Vitamin C necessary for collagen and tissue repair.
When is a bed sore considered a medical emergency? If the wound shows exposed bone or muscle, or signs of severe infection like fever, seek emergency care.
Conclusion
Managing pressure ulcers requires patience, a strict hygiene routine, and a focus on overall health. By combining medical techniques with nutritional support and emotional care, you can help your loved ones recover. Consistent care and early detection are the keys to maintaining skin integrity and ensuring long-term patient comfort. Taking these proactive steps allows for a more manageable recovery process for both the patient and the caregiver at home.















Write a comment ...